This is the title of a recent paper by the author Hernandez and Hong (2024). This article provides an excellent review of how drugs are reimbursed in the United States and who the major players are.I've provided a brief summary below, but please read full text.
players
- manufacturer Research, develop and bring new medicines to market.
- wholesaler Acts as a pharmaceutical distributor. Wholesalers purchase drugs from manufacturers and distribute them to pharmacies and health care providers.
- pharmacy Dispensing self-administered prescription medications to patients. Types of pharmacies include retail, mail order, online, specialty, and institutional.
- healthcare institutions Prescribe all medications and administer medications that require supervision by a health care professional (e.g., infusions, certain injections).
- patient Are consumers of medicines from a healthcare provider (physician-administered) or pharmacy (self-administered).
- Health plan or insurance company (also called payer) Provides medical and pharmacy services to its members. Private insurance is funded by employers and employees; public insurance (e.g., Medicare, Medicaid) is funded by taxes. Drugs dispensed to patients by outpatient pharmacies are covered by the policy's pharmacy benefit, while drugs administered by a provider are covered by the medical benefit. Health plans or insurance companies often subcontract pharmacy benefit management to a pharmacy benefit manager (PBM). A health plan or insurance company is also called a payer.
- PBM Manage drug benefits for insurance policies and design formularies, negotiate discounts with manufacturers, establish pharmacy networks, negotiate contracts with pharmacies or pharmacy services management organizations, and process and pay claims.
- Group Purchasing Organization (GPO) A buying syndicate pools the purchasing power of its members, allowing them to negotiate better discounts than they could obtain individually. GPOs include health systems, clinics, specialty pharmacies, retail pharmacies and PBMs.
- Pharmaceutical services administrative agency Represents independent pharmacy management and negotiates contracts with PBMs. Some Pharmaceutical Services Regulators are affiliated with or part of wholesalers.
Covering the financial flow of medicines Pharmacy Benefits
The chart below summarizes payments among these players for the medications patients receive through pharmacies. The pharmacy can be a standard independent pharmacy (e.g., CVS, Walgreens), a pharmacy within a hospital, or even a mail-order pharmacy.
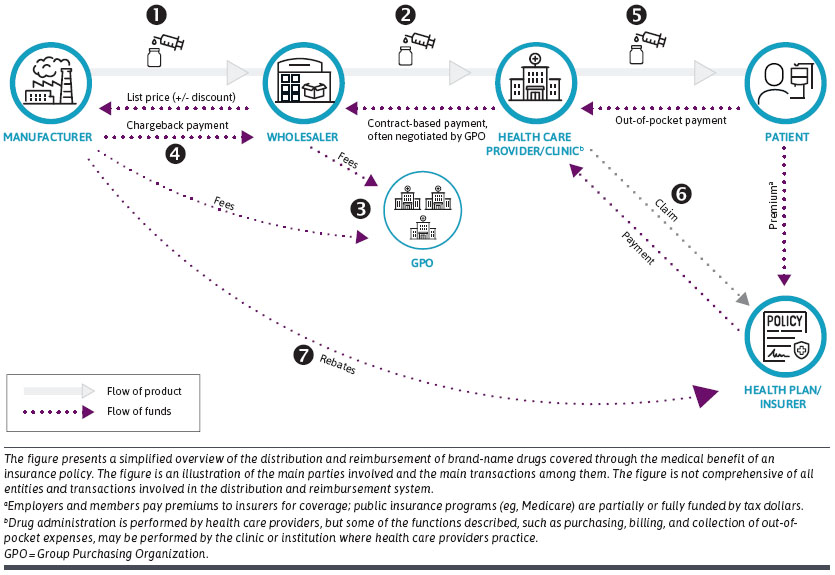
Covering the financial flow of medicines medical benefits
Here, instead of the pharmacy delivering the medication to the patient, the healthcare provider delivers the medication. These providers can receive reimbursement for the cost of the drug administered and for professional services provided to administer the drug.
expect
The article also identifies some key themes:
- Drug prices have been rising in recent years, but rebates are even higher.
- Federal drug price negotiations begin with Inflation Reduction Act (IRA)
- Increase vertical integration with insurance companies buying PBMs and create PBM-owned GPOs
- Health plans are increasingly using specialty provider-administered medicines through “white bagging” (having specialty pharmacies dispense medications and shipping them to providers) or “brown bagging” (letting specialty pharmacies dispense medications to patients). Drug Shift Pharmacy Benefit. brought to provider for management)



