According to some recent reports, the financial situation of hospitals in 2022 looks very poor. Government cash injections from COVID-19, which were helpful during the pandemic, have largely disappeared. At the same time, labor and supply costs have risen.Adding to these financial pressures are Recent Rise in RSV Cases.
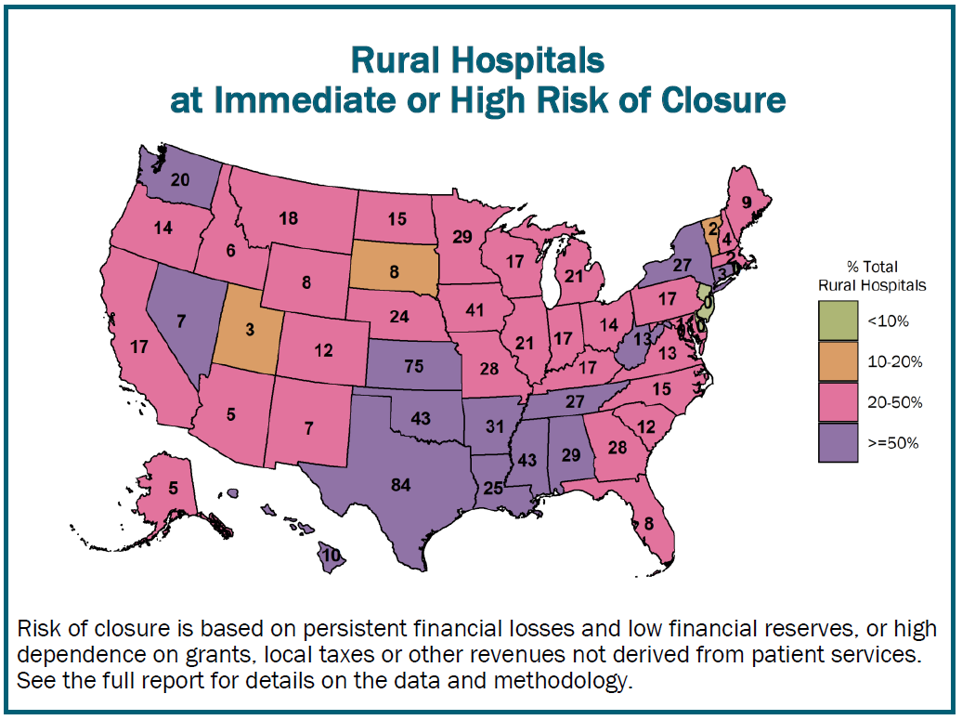
according to a Report of the American Hospital Association, hospital profit margins are down 37% from pre-pandemic (2019) levels. Additionally, more than half of hospitals expect negative profit margins.
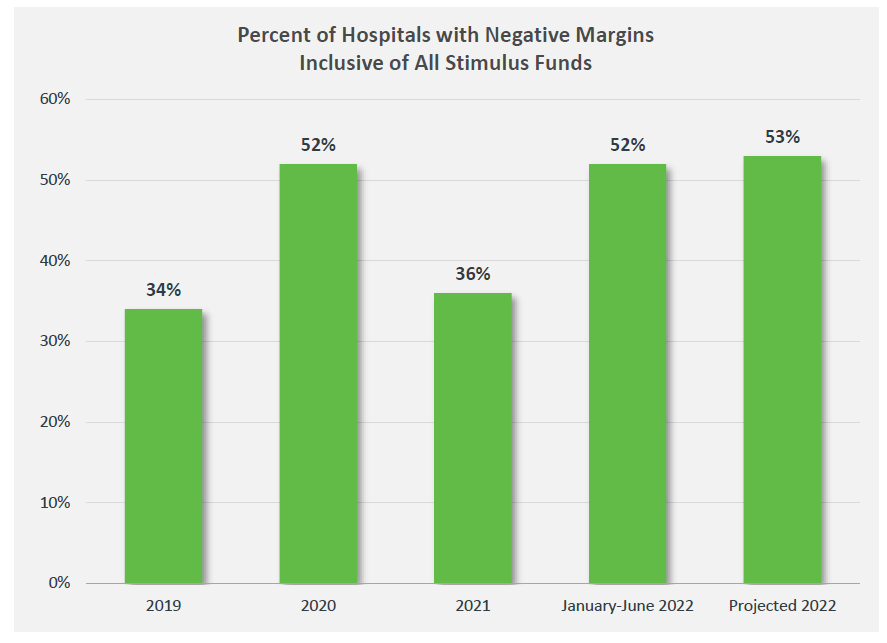
Rural hospitals are also struggling.One Report from the Center for Healthcare Quality and Payment Reform (Miller 2020) Many rural hospitals were found to be in poor financial condition. More than 800 rural hospitals (40% of the country’s total) are at risk of closure in the near future. This is partly because rural hospitals tend to be smaller due to lower population densities in rural areas. The report states:
Average costs for emergency room visits, hospital days, laboratory tests, imaging studies, and primary care visits are inherently higher in small rural hospitals and clinics than in larger hospitals because the lowest levels of staff and equipment are required to provide each of these services regardless of How many patients need to use them. For example, a hospital emergency department must have at least one doctor on call 24/7 to respond to injuries and medical emergencies quickly and efficiently, regardless of how many patients actually present to the emergency department. Smaller communities will have fewer ED visits, but the cost of ED spare capacity will be the same, so the average cost per visit will be higher.
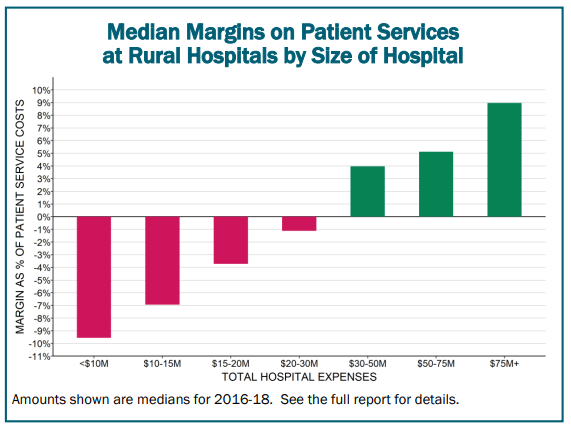
Unsurprisingly, the smallest hospitals generally had the lowest hospital profit margins.
How might hospitals respond to these financial constraints?Based on an article from Robinson et al. (2011)the answer may depend on the particular market structure in which the hospital operates.
…Confronted with a gap between Medicare payments and projected costs, hospitals in concentrated markets focus on raising prices to private insurers, while hospitals in competitive markets focus on cutting costs…
Policymakers may need to walk a tightrope on cost containment and shifting costs to private payers.
Public policy aims to limit Medicare spending and encourage provider coordination. Whether these two strategies will result in lower overall cost trends, or an accelerated cost shift from public to private insurers remains an open question.



